Dr Katie Knight | Dr Dani Hall
How not to be burned by Burns – Part 1: Minor burns and scalds
It’s 4 o’clock on a Friday afternoon. You’re working in the Paediatric Emergency Department gazing longingly at the clock. You’re just thinking about having a tea break when the triage nurse asks you to have a look at Maisie.
Maisie is one and a half. An hour ago her mum made a large cup of tea and turned her back for a millisecond to get a biscuit out the cupboard. Quick as a flash, Maisie reached up to the counter and made a grab for the tea which spilled all down her front. Mum panicked, scooped Maisie up into her arms and drove like mad to your Emergency Department. You ask Mum if she gave any first aid and she looks at you in horror and says no, she just panicked and came straight here. What should you do?
Maisie needs two things immediately – proper pain relief and first aid. At the minimum she’ll need simple analgesia such as paracetamol and ibuprofen – but you should have a low threshold for something stronger like oral morphine or intranasal diamorphine or fentanyl. And of course, never forget that distraction is an incredible addition to your analgesic.
When we talk about first aid in burns, the most important thing to do is apply cool running water to the burn for 20 minutes. This is because:
- it significantly reduce pain and oedema
- it decreases the inflammatory response and so reduces the fluid required for resuscitation
- it will improve the speed of wound healing and reduce scarring
When tissue suffers a burn, proteins are denatured and capillaries are dilated in response to inflammatory mediators. There is also a breakdown of intracellular ground substance and the spaces between endothelial cells open up… all of these factors make for leaky capillaries, which lose fluid and albumin into the interstitial space, causing oedema. None of this is good for healing!

So, stopping the burning process is really important.
You can still make a difference with good first aid within 3 hours of the injury – so if the parents only managed 5 minutes at home before rushing to hospital, make up that extra 15 minutes in ED!
Despite liberally dousing Maisie with cold water, the two of you have made friends. She seems well analgesed and you’re happy you’ve stopped the burns process as much as possible with your first aid, so now you need to assess the burn.
How do we assess burns? First we assess depth.

Burns can be categorised into three groups:
Superficial burns – these only affect the topmost layer of skin and cause erythema. They heal well with simple first aid. Most have us have had a superficial burn: the classic example is sunburn.
Partial thickness burns extend down into the epidermis. They can be further categorised into superficial partial thickness, mid-dermal partial thickness and deep dermal partial thickness. They classically blister.
Full thickness burns. Now these go beyond the dermis down to deeper structures such as nerves and muscle.
Let’s look at some examples…
Partial Thickness

This child’s skin has blistered which makes it (PROBABLY) a partial thickness burn. But the problem is we can’t assess the skin UNDERNEATH the blister. Classic thinking was that blistered burns should be left alone but now we know that blisters must be removed because:
- it allows assessment of burn wound bed
- non-viable tissue is removed
- there is a risk of blister infection
- it relieves pain in tense blisters
- it reduces restriction of movement of joints
Any burn blisters bigger than the patient’s little fingernail should be ‘deroofed’. One deroofed, the burn wound should be dressed with a non-adherent dressing.
If you haven’t seen a blister being deroofed, it’s worth asking the nurses if you can watch the procedure so you know what is involved. The child HAS to have proper analgesia first, as it is potentially very painful (blister gets popped and drained, and all the blistered skin removed with tweezers and/or vigorously wiping the area with wet gauze).
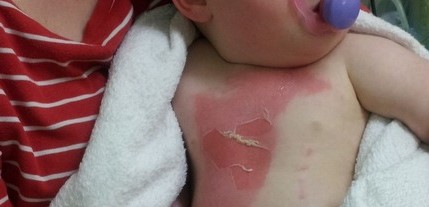
Superficial dermal partial thickness
Under this blister, you can see the child has a superficial dermal partia l thickness burn. It has a pink wound bed, is moist with moderate exudate and if you check the capillary refill (which you must do), it is brisk.
l thickness burn. It has a pink wound bed, is moist with moderate exudate and if you check the capillary refill (which you must do), it is brisk.
The burn is very painful and sensitive to air and temperature but with good dressings will heal in 7-10 days.
Mid dermal partial thickness
Mid dermal partial thickness burns are deeper, but the base is still viable and pink (varying from light pink to dark pink). Some, but not all, nerve endings remain intact so they are painful but often not as painful as the superficial partial thickness burns. Some capillaries are also still viable so there is still capillary return but it’s slower than in superficial partial thickness burns.
Deep dermal partial thickness
This child has a deep dermal burn. It is less painful as more nerves have become destroyed, tending to be sensitive to deep pressure but not pinprick. It looks cherry red or pale white in colour and has really sluggish capillary refill. It has ‘staining’ of the burn due to coagulated blood vessels and can be wet, waxy or dry compared to a superficial partial thickness burn. These take over 6 weeks to heal and is likely to scar and is often due to a chemical burn, contact burn or flame.
Full thickness
This is a full thickness burn. It involves all the layers of the skin and subcutaneous tissue, with involvement of underlying fascia, muscle, bone, or other structures, resulting from prolonged exposure
It looks white or cream, there may be a black or brown waxy appearance with visible thrombosed vessels. It is usually painless (because the nerves have been destroyed) and is most often due to flames, contact burns or chemical burns. Skin grafts are normally needed, and scarring is very likely.
A word on Child Protection
As with all injuries in children, burns must get your alarm bells ringing for child protection concerns. Does the history given fit the appearance of the burn? Could this have been non-accidental? Was the child being supervised appropriately, and was there any delay in presentation?
After depth, assess total size of burn
There are several ways of assessing the size of a burn. Lund and Browder charts give us different body surface area percentages of each bit of the body depending on the child’s age. There are also some great apps around (like Mersey Burns) – you enter in the child’s age, colour in the burned bits on a body map and hey presto, it calculates a percentage body surface area.


But my favourite method is using the palm and adducted fingers of the child ’s hand (not your hand!) as 1% total body surface area.
’s hand (not your hand!) as 1% total body surface area.

But don’t forget, DON’T count erythema in your burns calculations! Barbie has zero % TBSA burns (but is going to need a LOT of Aloe Vera to take away the sting).
Anyway, I seem to have digressed. Back to Maisie…
Now that the blister on Maisie’s chest has been deroofed, you can see the scalds are superficial partial thickness burns to the chest and face, in total around 1% body surface area. You take some photos because you have a feeling the regional burns unit will need to follow her up.
The burns on her chest need dressing with a non-adherent dressing and lots of gauze (burns ooze a lot) and then an adherent dressing and crepe bandage to go over the top. Scalds on the face often have to be left undressed depending on their position, as it can be tricky to bandage this area.
Referring to specialist burns networks
Each Burns Network will have their own referral pathway (this is the London and South East Burns Network one). Although Maisie doesn’t have any deep dermal or full thickness burns, and although her scald is not greater than 1% TBSA, she does have burns to the face. Liaising with the regional burns centre, they say they’ll see Maisie tomorrow.
Maisie can go home – but what safety netting advice does her mum need to hear?
Symptoms of Toxic Shock Syndrome
The rare, but very serious potential complication of any burn – no matter how small – is Toxic Shock Syndrome (TSS).
Toxic Shock Syndrome (TSS) is due to Staph Aureus producing TSS Toxin-1 (exotoxin) resulting in a massive cytokine ‘storm’. It classically presents in young children with small burns and the mortality is massive, up to 50%. Children with burns are particularly at risk of toxic shock because the burn presents a breach in the skin – the burn is colonised with staph aureus and is the ideal environment for toxin formation because it’s aerobic with a neutral pH. TSS classically affects small superficial partial thickness burns, like Maisie’s.
Maisie’s mum needs to look out for symptoms of fever, vomiting, diarrhoea, malaise and rash – if Maisie has any of these symptoms she has to get to the Emergency Department ASAP. These particular symptoms related to the prodromal period of TSS, which lasts 1-2 days and often presents 2-4 days after the burn, before the next stage of symptoms of skin desquamation, confusion and coma. The burn usually appears clean and not infected – but this is serious stuff because if it’s not recognised early, it leads to septic shock.
As well as being shocked, the child’s bloods in TSS often show a lymphopaenia, neutropaenia, low platelets and low sodium. If you suspect TSS, you MUST give broad spectrum intravenous antibiotics, fluid resuscitation and get right on the phone to PICU.
Watch this space for Part 2 – How not to be burned by Burns: Major burns
Katie Knight, Paediatric Emergency Medicine Registrar; Dani Hall, Consultant in Paediatric Emergency Medicine, Evelina London Children’s Hospital

What an excellent resource I am a children’s community nurse abs clinical lead this is excellent for training purposes for within the service
Excellent post. I have read conflicting evidence on this. Curious to know your thoughts on this – https://first10em.com/should-i-debride-burn-blisters/
Thanks
Lakshay